- Startseite
- Publikationen
- GIGA Focus
- COVID-19 in Latin America: Where We Stand and What Is to Come
GIGA Focus Lateinamerika
COVID-19 in Lateinamerika: wo wir stehen und was auf uns zukommt
Nummer 5 | 2021 | ISSN: 1862-3573
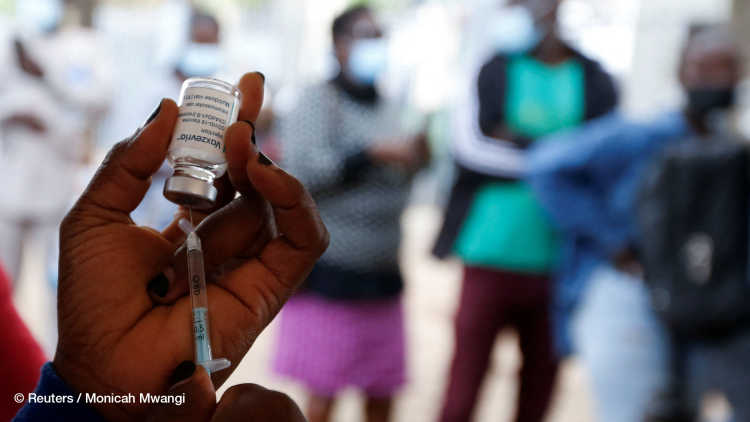
Da die Infektionsraten in großen Teilen Lateinamerikas zurückgehen, scheint die Region eine Atempause von der COVID-19-Pandemie zu bekommen. Der Zugang zu Impfstoffen ist jedoch sowohl innerhalb der einzelnen Länder als auch zwischen ihnen ungleich verteilt, und die Immunisierungsraten durch Impfungen sind sehr unterschiedlich. In Verbindung mit dem Auftreten der hochansteckenden Delta-Variante sind neue epidemiologische und politische Herausforderungen zu bewältigen.
Mit 45 Millionen registrierten Infektionen und fast einem Drittel aller COVID-19-bedingten Todesfälle weltweit ist Lateinamerika zu einem globalen Hotspot der Pandemie geworden.
Chile und Costa Rica haben höhere Impfraten als Deutschland oder die Vereinigten Staaten, aber die Hälfte der lateinamerikanischen Bevölkerung hat noch immer nicht ihre erste Impfung erhalten. Zu Hilfe kommt dabei nun die große Zahl der Menschen, die durch eine frühere COVID-19-Infektion eine gewisse Immunität erworben hat – und die weit über die in den offiziellen Statistiken erfassten Fälle hinausgeht.
Die Impfdiplomatie hat ihren Charakter geändert. Ursprünglich war Lateinamerika auf Impfstofflieferungen aus China, Indien und Russland angewiesen. Inzwischen sind die USA und die multilaterale COVAX-Initiative zu den größten Gebern avanciert. Die Politik wird sich auf die daraus resultierende Mischung von Impfstoffen mit unterschiedlicher Wirksamkeit und unterschiedlicher internationaler Anerkennung einstellen müssen.
Um die externe Abhängigkeit zu verringern, muss die Region ihre Kapazitäten für die Entwicklung und Massenproduktion von Impfstoffen, Diagnosegeräten und mRNA-Technologie ausbauen. Die in Kuba entwickelten Impfstoffe können Teil des Impfstoffportfolios werden, das der Kontinent in den kommenden Jahren benötigen wird.
Die Pandemie hat die strukturellen Schwächen der Region aufgedeckt. Die Mittel für die öffentliche Gesundheit müssen aufgestockt werden; die während der Pandemie getroffenen sozialpolitischen Ad-hoc-Maßnahmen sollten genutzt werden, um die sozialen Sicherheitsnetze auf Dauer tragfähiger und integrativer zu machen.
Fazit
Um die Pandemie einzudämmen, ist eine intensive Impfkampagne weiterhin unerlässlich. Da die Immunität – sei es aufgrund einer früheren Infektion oder einer Impfung – mit der Zeit nachlässt, werden Impfungen in die routinemäßige Gesundheitsvorsorge zu integrieren sein. Die verstärkte Zusammenarbeit über ideologische Links-Rechts-Dichotomien hinweg bei der epidemiologischen Diagnose, der Forschung, der Impfung und der Gesundheitsversorgung, sollte sowohl in der Region als auch bei den internationalen Partnern zu einer Priorität werden.
The Latin American Drama: Is the Worst Over?
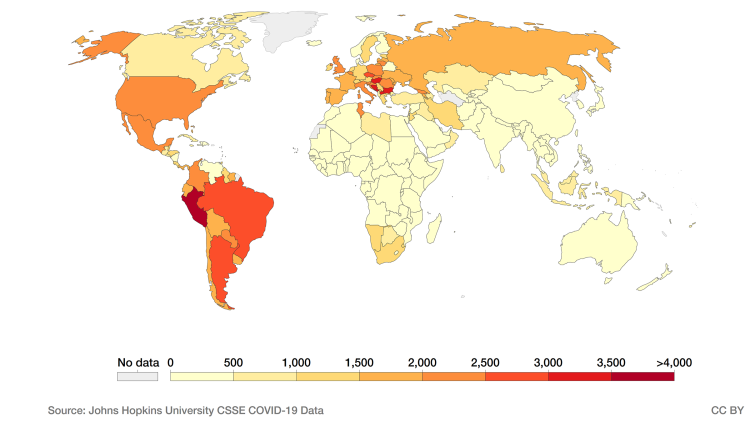
Despite being home to just 8.4 per cent of the world’s population, Latin America and the Caribbean has accounted for almost one-third of COVID-19-related deaths to date. This includes the world’s second-highest death toll on the country level (Brazil) and the world’s highest registered rate of deaths per capita (Peru; see Figure 1). The tragic milestone of a million deaths regionally was passed as early as May 2021.
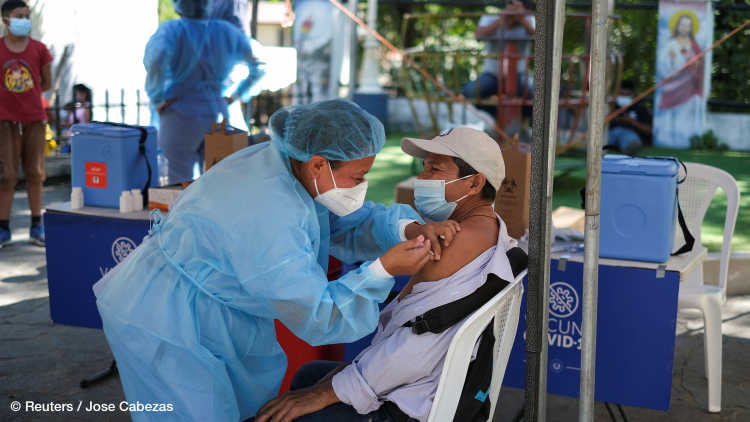
The horrendous death toll in Latin America and the Caribbean comes despite a population with a median age of 31, and hence much younger than that of the United States (median age 38.5) or Europe (42.5). The case of Peru – which for years had some of the highest economic growth rates on the continent – highlights that the death toll is no mere function of gross domestic product. Instead, the pandemic has brutally exposed the region’s structural weaknesses: strained and underfunded healthcare systems, late and limited access to vaccines, deep-seated social inequalities, extensive informal-labour practices, unhealthy diets leading to widespread obesity, insufficient state capacity, and incoherent policies have all contributed to this painful outcome.
Beyond the epidemiological drama, the economic and social fallout from disrupted global trade and travel as well as from lockdown measures has been enormous, from steep economic decline, to psychological suffering, to lost educational potential. A recent study estimates that 22 million more people fell into poverty in the region in 2020, with a significant impact on children (ECLAC and PAHO 2021: 3). It also stressed that in what is the world’s most unequal region “socioeconomic vulnerability is highly correlated with the severity of COVID-19 infection and mortality” (ECLAC and PAHO 2021: 18).
The COVID-19 pandemic has also shown that early advances are not the same as long-term success. Israel, the United Kingdom, and the US had been frontrunners in the vaccination drive; by late 2021, however, not only have their vaccination rates become stagnant but their COVID-19 infections per capita are higher than those of South America. Certainly, significant undercounting due to insufficient testing or test avoidance must be taken into account here. But still: while in Israel, the UK, and the US infection rates have gone up since summer 2021, in South America reported infection, hospitalisation, and death rates have all been in decline. There are three main factors likely explaining this trend:
The seasonal effect, since the Southern Hemisphere is now past winter season.
The progress of vaccination campaigns. Most Latin American countries have by now attained vaccination coverage rates of around 30 to 60 per cent of their populations, which is far higher than in other tropical regions such as sub-Saharan Africa.
A large share of the population have acquired some level of immunity from having experienced infection, whether diagnosed or not.
However, the highly contagious Delta variant of SARS-CoV-2 – a so-called variant of concern (VOC) which has swept most of the world already – is only now making its full entry into South America. It arrived earlier this summer in the Caribbean, which in its wake would see soaring infection rates. Barbados currently tops global tables with a seven-day incidence rate of more than 700 infections per 100,000 people.
So how much light is there at the end of the tunnel for Latin America? Is the worst over, really? To tackle this question we look at the uneven vaccination process in the region; at the heterogenous levels of past infections conferring some level of immunity; at the delayed arrival of the Delta variant in parts of the region; and, at the complex mix of vaccines applied and the implications hereof. We then address the need to strengthen pandemic preparedness to overcome external dependence, before finally identifying necessary steps towards rectifying the societal and economic damage the pandemic has wreaked regionally.
Large-Scale but Uneven Vaccination
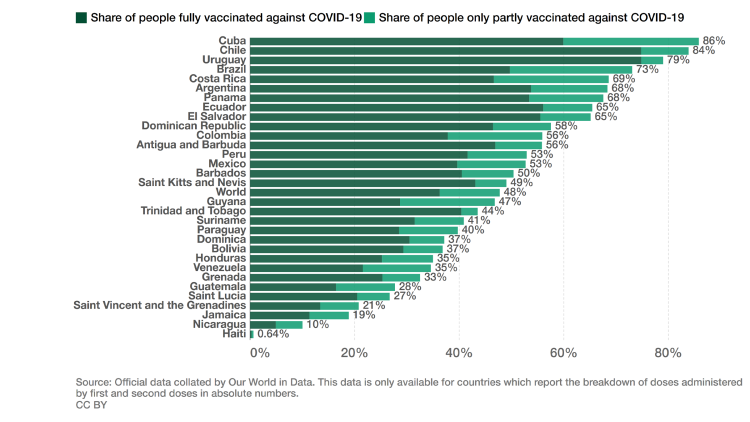
The absolute scarcity of vaccines marking the initial phase of the pandemic has since given way to a highly uneven process of vaccination in the region – between countries, within countries, and also with regards to the types of vaccines available. In the last few months, almost all Latin American countries have significantly advanced their vaccination programmes (see Figure 2 below). But it is worth distinguishing between three sub-regions here:
Across South America, almost two-thirds of the population have received at least their first shot; only Venezuela’s vaccination rate is below the global average.
In Central America the picture is mixed: significant progress in Costa Rica, El Salvador, and Panama; low vaccination rates in Guatemala, Honduras, and Nicaragua; in Mexico, a middle ground has been reached, being almost on par with Colombia and Peru but clearly below South America’s leaders Argentina, Brazil, Chile, and Uruguay.
In the Caribbean, initially clever vaccine diplomacy made a number of states vaccination pioneers (Hoffmann 2021). However, these campaigns soon stagnated; by now, vaccination rates largely trail behind those on the Latin American mainland. Cuba is a notable exception: it started vaccination later than others, but almost 90 per cent of the population have received at least a first dose.
In many places, vaccine availability is still a bottleneck. Another issue – also very unevenly distributed – is vaccine hesitancy. In Brazil, for instance, public-health institutions have a long-standing reputation for social progress, and over the decades vaccinations have acquired broad acceptance. This has prevailed over social media disinformation and the negationist attitude of the federal government. The metropoles Rio de Janeiro and São Paulo by now boast higher vaccination rates than Berlin or New York.
Nevertheless in other countries, including many in the Caribbean, health authorities are battling with vaccine scepticism, even as the Delta variant sweeps the region with force. In the small island state of Dominica, for instance, as early as 1 April 2021 some 25 per cent of the population had received their first jab, putting the country at the vanguard. However since then the vaccination campaign has advanced at snail’s pace: standing at less than 35 per cent by 1 October 2021. Dr. Carissa Etienne, Director of the Pan American Health Organization (PAHO) and herself a native of Dominica, recently noted: “Even when vaccines are available, persons are not coming forward” (PAHO 2021).
In Jamaica, the vaccination rate is lower still. Less than 10 per cent of the population have been fully vaccinated. According to one 2020 survey, 72 per cent of Jamaicans reportedly said they would not accept a COVID-19 vaccine (cited in CARPHA 2021: 2). However, surveys fail to provide satisfactory explanations. In the one carried out by the Caribbean Public Health Agency, respondents most often offered the standard answers: that they were concerned about possible side effects; did not know enough about the vaccine; thought the vaccine was developed too quickly (CARPHA 2021: 11). But in none of this – nor in its exposure to social media – does the region differ from the rest of the world. Instead, it seems likely that part of the mistrust is rooted in a history of racialised, colonial public health – including unethical healthcare research among Afro-descendent populations.
The Delayed Entry of the Delta Variant
Since this summer the Delta VOC’s predominance has been observed globally, however not (yet) in all of South America. In Colombia the Mu variant still dominates, in Bolivia the Gamma variant, while in Peru the Lambda variant maintains a strong presence. Whether these have delayed the rise of the Delta variant or whether its late introduction is simply a matter of reduced international connectivity remains a matter of debate. Nonetheless, there is little doubt that the increased transmissibility of the Delta variant will lead to its dominance in those countries eventually.
In Mexico, where the Delta variant became dominant over the course of this summer, COVID-19 infection rates have gone up – but not dramatically, and not for long. Argentine health minister Carla Vizzotti warned that it will be impossible to prevent the Delta variant from circulating in the country; indeed, it has come to represent 50 per cent of cases in the latest samples. In Brazil, many feared that the Delta variant would produce another wave of devastation in a country which has already mourned 600,000 dead. However, even with the Delta variant fully dominating by now and despite a relaxing of social-distancing measures so far no major increase in infection rates has been seen.
This is all the more remarkable as in the Caribbean the picture is the absolute opposite. The latter had passed impressively lightly through the early waves of the pandemic compared to mainland Latin America. However, this changed when the Delta VOC reached the Caribbean’s islands this summer. The first country hit was Cuba, where spiralling infection rates brought the island’s healthcare system to the brink of collapse. More recently, it has been the island states of the anglophone Caribbean seeing an explosion of cases – battering their healthcare systems and putting them among the countries with the world’s highest per capita incidences of infection (Figure 3).
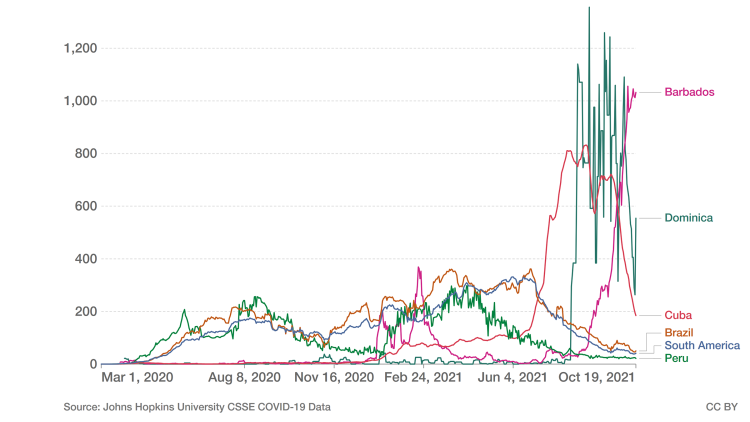
Partial Immunity through Past Infection
So what explains these regional differences? Combined with insufficient vaccination rates, the crucial difference is probably the Caribbean’s comparatively low exposure to the virus in the first year and a half of the pandemic. In both Central and South America in contrast, the raging pandemic left hundreds of thousands dead, and millions infected. Brazil, for instance, has reported almost 20 million confirmed cases as of October 2021, more than 10 per cent of the country’s total population. This may just be the tip of the iceberg, given the high proportion of asymptomatic or mild infections (estimated at around 80 per cent in most studies) and low testing capacities. In consequence, it is very likely that in Brazil – as in many other Latin American countries too – COVID-19 infections have been much more widespread than official data can capture.
The rate of undetected infections will be particularly high among the young, as well as in rural and poor urban settings where insufficient healthcare infrastructures likely intersect with test avoidance since mandatory quarantine is perceived as incompatible with the income imperatives of day labourers or street vendors. Consequently, past COVID-19 infections have mediated partial immunity, complementing the advent of vaccine programmes – but at a desperate cost in terms of both individual suffering and societal disruption.
The way to know more about the pervasiveness of past infections is studies on “seropositivity” – that is, blood analyses showing antibodies from past infections no matter whether one was symptomatic or not, and regardless of whether the case was reported or not. Unfortunately, such studies are not systematically available for the whole continent. But some case studies do show high rates of “hidden infections.” For instance, a March 2021 study in northern Peru’s San Martín region showed an overall 59.0 percent seroprevalence, diverging substantially from reported incidence (Moreira-Soto et al. 2021). However, earlier studies from 2020 reporting stunning seroprevalence rates of around 70 per cent from Iquitos in the Peruvian Amazon (Alvarez-Antonio et al. 2021) or Manaus in the Brazilian Amazon (Buss et al. 2021) have to be taken with caution. Antibody tests used in Latin America frequently are neither designed nor validated for usage in tropical regions and can lead to false positives, as shown in Moreira-Soto et al. (2021) and Yadouleton et al. (2021) (Drexler a co-author in both). This may in part explain renewed outbreaks in Iquitos and Manaus, when some thought herd immunity had already been reached.
Despite these caveats, in Latin America (partial) immunity likely not only comes from vaccination but also from the high rates of those who have experienced COVID-19 infection – symptomatic or not, detected or not. This also helps to explain why the arrival of the Delta variant has caused such havoc in the Caribbean: Here, initially, the pandemic had been kept at bay better than elsewhere. Dominica, for instance, did not have to report a single fatality for more than a year and a half after the outbreak of the pandemic, and other anglophone island states had similarly impressive low infection and death rates.
Precisely because of that success, in the Caribbean the Delta variant encountered a population in which only the vaccinated had some immunity, and very few of the non-vaccinated. It should be noted that, luckily, across all of Latin America and the Caribbean high numbers of infections do not translate into similarly high fatality rates as those witnessed during the early phases of the pandemic. This is due to increased vaccination of the elderly and other at-risk population strata.
A Complex Mix of Vaccines
Understanding the course of the pandemic also requires scrutinising which vaccines have been used in the region. They can be split into four categories:
The vectored vaccines like those from AstraZeneca, Johnson & Johnson, or the Russian Sputnik (adenovirus vectors carrying the gene encoding the spike surface protein of the new coronavirus)
The mRNA vaccines like those from Pfizer/BioNTech and Moderna (a modified messenger RNA encoding the spike protein)
The inactivated vaccines like SinoVac and Sinopharm (relying on cultivated SARS-CoV-2 that is chemically inactivated, for example by formaldehyde)
The protein-subunit-based vaccines like both of Cuba’s, Abdala and Soberana (relying on the receptor-binding domain of the spike protein, in the case of Soberana coupled to tetanus toxoid to increase immunogenicity).
Each of these vaccine formulations has its advantages and disadvantages in the Latin American context. The mRNA vaccines have shown extremely high efficacy in preventing disease, but require storage at very low temperatures. During the early days of the pandemic, those mRNA vaccines were neither available to nor logistically manageable in most countries of the region. Sputnik was offered by the Russian authorities early on, but geopolitical negotiations limited availability and did not allow widespread usage in the region. Inactivated vaccines produced in China were available and affordable and thus formed the backbone of the early vaccination programmes. Both Cuban vaccines rely on relatively simpler technology, and as such they are fairly easy to produce, to store, and to administer – even if they require multiple shots each.
All these vaccines thus afford some protection against COVID-19, but at different levels of efficacy. In the Latin American context, this became clearest when Chile – which until then had 93 per cent reliance on the SinoVac vaccine – suffered yet another wave of infections this April despite what was back then Latin America’s highest vaccination coverage (50 per cent of the population having received at least one dose). This may well be associated with relatively lower efficacy of inactivated vaccines due to changes in protein structure caused by the chemicals used for virus inactivation, affording reduced immunogenicity. To contain this deadly wave the country had to return to non-pharmaceutical interventions such as lockdown measures, which in turn contributed to the severe economic crisis the country – as all of Latin America – has been suffering in the wake of the pandemic. As of late 2021, mRNA and vectored live vaccines have become more widely available and most countries have come to using a broad spectrum of vaccine formulations, mixing them successfully.
Vaccines: From Donations to Domestic Production
During 2020 and early 2021, Europe and the US secured the bulk of the vaccines produced by Western companies for their own populations, with most countries in Latin America turning to China, India, and Russia instead. Over time, however, vaccine diplomacy has changed colours. With its domestic vaccination campaign having stagnated, Washington is passing on millions of excess doses to other countries. The US has by now become the prime vaccine donor to Latin America (Harrison 2021). Beyond donations, Latin American countries have also sought direct procurement from producers as well as acquisition via the multilateral COVAX facility in its different forms.
COVAX, to which Europe, the US, and other developed nations pledged billions of euros, initially got off to a slow start. For supplies, it largely relied on India’s vaccine production; with the latter’s own massive COVID-19 outbreak in April, however, all vaccine exports were halted to cater to domestic demand first. Even if COVAX, working together with the PAHO, has distributed more than 20 million vaccine doses to Latin America and the Caribbean this is still far below what was originally planned and pledged. Despite deliveries now increasing, disappointment with COVAX still weighs heavily throughout the region. One consequence is that the PAHO has struck separate deals to buy millions of Chinese Sinopharm and Sinovac vaccine doses, as well as AstraZeneca ones too.
Initiatives for the local development of COVID-19 vaccines or the licenced production of existing vaccines have proven to be more complex than initially hoped. However, a Mexican-Argentine collaborative project with AstraZeneca reported to have shipped its first batch of a million locally produced vaccines to Argentina, Belize, Bolivia, and Paraguay in June 2021 (Navarro 2021). Cuba’s vaccines are a different case besides, as they are not produced under licence from international companies but are original developments by the island’s biotech sector – a remarkable accomplishment given the economic constraints of the country and the fact that much richer states and deep-pocketed global pharma companies failed to achieve this.
However, as mass production of the vaccine took longer than planned, the island started its vaccination campaign late – paying a heavy price for that. The arrival of the Delta variant in June 2021 led to a surge of infections wreaking havoc on the Cuba’s healthcare sector, traditionally the country’s pride. If Cuba initially gained international repute by sending doctors and health workers abroad to fight the pandemic, it now had to seek medical and other humanitarian support from outside.
While Cuba’s vaccines have yet to receive World Health Organization recognition, they have stood the test of practical implementation. Once the island’s vaccination campaign got under way it gradually brought the curve of infections down. Efficacy in the face of the Delta variant may eventually be less than the 90 per cent officially announced following clinical trials, but the Cuban vaccines have clearly been instrumental in getting the pandemic under control.
Cuba also became the world’s first country to vaccinate children aged two and over. By the end of 2021, the island will likely have fully vaccinated 90 per cent of its population. With domestic demand covered, first shipments of Cuban vaccines have been exported to Venezuela and Vietnam. While they probably will not get recognition in Europe or the US any time soon, Cuban vaccines can be a helpful low-cost addition in the vaccination campaigns in Latin America, and in the Global South more generally.
However, Latin America will also need to expand its own capacity to develop and produce vaccines. The PAHO has selected two biomedical centres in Argentina and Brazil as regional hubs to develop and produce mRNA vaccines. In mid-October 2021 Mexico signed a deal with Russia to produce the Sputnik vaccine in state laboratories. Pfizer/BioNTech announced commencing production together with Brazil’s Eurofarma corporation, with at least 100 million doses annually projected for distribution in the region (Burger and Mishra 2021).
What Is to Be Done?
It may be that most of Latin America indeed has passed through the worst: The drama of infections spiralling out of control, hospitals being overrun, and a death toll measured in the hundred thousands may not see a repeat. However we do not know if new SARS-CoV-2 mutations will continue to thrive among partially immune populations, as some studies suggest (Baj et al. 2021). There is much about the new coronavirus we do not yet fully understand.
Regardless, the pandemic is far from over. It will have lasting effects on people’s health still difficult to assess. Non-pharmaceutical interventions – from mask-wearing to social-distancing measures – are likely to still be indispensable in many places. Opening up once again to travel and tourism entails the risk of reinvigorating infection curves. Moreover, the pandemic has created economic and social disruptions, sharpened socio-economic inequalities, increased gender-based violence, and brought about a range of other consequences that also weigh heavily on the region’s future. Not only Latin America’s healthcare systems but, more broadly, the region’s societies and economies will be struggling with COVID-19 for years – if not decades – to come.
What we do know: immunity – whether through vaccination, past infection, or the combination of both – will not last forever. In the case of yellow fever, childhood infection gives permanent immunity, and the effect of a single-shot jab is thought to last a lifetime. In contrast, COVID-19 immunity will wane sooner or later. Since we know this, we can prepare for it in advance. Vaccination boosters will have to become part of routine healthcare provision if we are to avoid new rounds of deadly outbreaks – and the policy measures needed to cope with them.
New medication is being developed, but as of now no magic bullet is in sight. Molnupiravir, which recently sought emergency-use authorisation in the US, may reduce the risk of hospitalisation or death significantly, but only if infection is detected at an early stage and medication is swiftly administered. Additionally, the drug’s safety profile is not fully understood yet. As with previous vaccines, rich countries may secure the first produced batches for themselves, and prices will likely be prohibitively high for much of Latin America’s population.
The pandemic has exposed crucial structural weaknesses that Latin American countries will need to address if they are to fare better in the future:
The chronic underfunding and dysfunctional structures of the public-health systems need to be overcome so that they can provide effective healthcare services to the citizenry at large, not only to the well-off.
The region will need to build up the ability to develop and mass-produce own vaccines, diagnostic equipment, and mRNA technology to reduce dependence on foreign providers.
Cooperation and scientific exchange within the region need to become swifter and better institutionalised, be it as part of or as complement to existing supranational schemes.
As vaccines are being produced in the region, trade in them should be eased. The Cuba-made vaccines should not be seen per ideological but rather per medical criteria. As such, they can form a vital part of the vaccine portfolio that the continent will need for many years to come.
Ad hoc social-policy measures that helped significantly expand coverage (Blofield et al. 2020) should not be shelved as soon as the sense of emergency recedes, rather seen as an opportunity to make permanent social safety nets more resilient and inclusive.
The severe drops seen in GDP and living standards need to be reversed by policies that indeed live up to the promise of “building back better” – that is, ones leading to more equitable and sustainable economies.
The pandemic has also underscored the importance of political stability, of personal integrity, and of a fact-based public discourse beyond short-term partisan gains or open disinformation.
International cooperation with actors from outside the region will continue to be important in many ways. In the early phases of the pandemic, COVAX fell short of expectations; as global vaccine production increases, however, it can be a key contributor to broad and equitable access to vaccines. This is true not only in the acute current crisis but also the near future. COVAX has the potential to bridge political divides that in times of a pandemic should step aside. For instance, the initiative has provided vaccines to Venezuela simultaneous to the US government explicitly excluding that country from its bilateral vaccine donations.
Research on COVID-19 and, more broadly, on infectious diseases is a task that needs strong engagement in transnational scientific cooperation and exchange. This includes pooled funding for joint research endeavours but also support for lab infrastructure and diagnostic capacities throughout Latin America. One such initiative is the “German-Latin American Centre of Infection & Epidemiology Research and Training” (GLACIER), in which both authors are involved and which aims at facilitating mutual learning and knowledge-sharing between universities and research centres in Germany, Cuba, Mexico, and throughout Central America.
Swiss author Friedrich Dürrenmatt, in the epilogue to his 1962 drama The Physicists, famously posited: “What concerns all, only all can solve. Each individual attempt to solve in isolation what concerns all must fail.” There is no national solution to a pandemic. As long as SARS-Cov2 remains unchecked in any part of the globe it will continue its process of mutation – potentially putting at risk the effectiveness of vaccinations and other measures. The fight against infectious diseases – and, more broadly, for global public health – is, then, a concern which “only all can solve.”
Fußnoten
Literatur
Alvarez-Antonio, Carlos et al. (2021), Seroprevalence of Anti-SARS-CoV-2 Antibodies in Iquitos, Peru in July and August, 2020: A Population-Based Study, in: The Lancet Global Health, 9, e925-e931, www.thelancet.com/action/showPdf?p ii=S2214--109X%2821%2900173-X (19 October 2021).
Baj, Andreina et al. (2021), Breakthrough Infections of E484K-Harboring SARS-CoV-2 Delta Variant, Lombardy, Italy, in: Emerg Infect Dis, 9 September, Epub ahead of print, wwwnc.cdc.gov/eid/article/27/12/21-1792_article (19 October 2021).
Blofield, Merike, Cecilia Giambruno, and Fernando Filgueira (2020), Policy Expansion in Compressed Time: Assessing the Speed, Breadth and Sufficiency of Post-COVID-19 Social Protection Measures in 10 Latin American Countries, ECLAC Social Policy Series 235, September, https://repositorio.cepal.org/bitstream/handle/11362/46016/4/S2000593_en.pdf (19 October 2021).
Burger, Ludwig, and Manas Mishra (2021), Brazil’s Eurofarma to make Pfizer COVID-19 Shots for Latin America, in: Reuters, 26 August, www.reuters.com/world/americas/pfizer-biontech-sign-deal-with-brazils-eurofarma-make-covid-19-shots-2021-08-26/ (19 October 2021).
Buss, Lewis F. et al. (2021), Three-Quarters Attack Rate of SARS-CoV-2 in the Brazilian Amazon During a Largely Unmitigated Epidemic, in: Science, 371 (6526), www.science.org/doi/pdf/10.1126/science.abe9728 (19 October 2021).
CARPHA (Caribbean Public Health Agency) (2021), COVID-19 Vaccine Acceptance Among Active Social Media Users in the Caribbean, Port of Spain: CARPHA, https://carpha.org/Portals/0/Publications/Summary%20Results%20of%20COVID-19%20Vaccine%20Acceptance%20Survey.pdf (19 October 2021).
ECLAC, and PAHO (Economic Commission for Latin America and the Caribbean, and Pan American Health Organization) (2021), The Prolongation of the Health Crisis and Its Impact on Health, The Economy and Social Development, COVID-19 report, Santiago de Chile, Washington, DC: ECLAC, and PAHO, 14 October, https://repositorio.cepal.org/bitstream/handle/11362/47302/1/S210059 3_en.pdf (19 October 2021).
Harrison, Chase (2021), Tracker: U.S. Vaccine Donations to Latin America, AS, and COA (Americas Society, and Council of the Americas), 30 September, www.as-coa.org/articles/tracker-us-vaccine-donations-latin-america (19 October 2021).
Hoffmann, Bert (2021), The Caribbean’s Skilful Vaccine Diplomacy, in: International Politics and Society, 31 March, www.ips-journal.eu/topics/foreign-and-security-policy/the-caribbeans-skilful-vaccine-diplomacy-5084/ (19 October 2021).
Moreira-Soto, Andrés et al. (2021), High SARS-CoV-2 Seroprevalence in Rural Peru, a cross-sectional population-based study, https://medrxiv.org/cgi/content/short/2021.10.19.21265219v1 (24 October 2021).
Navarro, Andrea (2021), Mexico Ships First Locally Made Astra Shots to Latin America, Bloomberg, 14 June, www.bloomberg.com/news/articles/2021-06-14/mexico-ships-first-locally-made-astra-shots-to-latin-america (19 October 2021).
Our World in Data (2021), Statistics and Research Coronavirus Pandemic (COVID-19), https://ourworldindata.org/coronavirus (19 October 2021).
PAHO (Pan American Health Organization) (2021), PAHO Director Appeals to Caribbean People to Get Vaccinated, Observe Protective Measures, 11 August, www.paho.org/en/news/11-8-2021-paho-director-appeals-caribbean-people-get-vaccinated-observe-protective-measures (19 October 2021).
Schmidt, Fabian et al. (2021), High Genetic Barrier to SARS-CoV-2 Polyclonal Neutralizing Antibody Escape, in: Nature, 20 September, Epub ahead of print, PMID: 34544114, www.nature.com/articles/s41586-021-04005-0 (19 October 2021).
Yadouleton, Anges et al. (2021), Limited Specificity of Serologic Tests for SARS-CoV-2 Antibody Detection, Benin, in: Emerg Infect Dis, January, 27, 1, 233–237, wwwnc.cdc.gov/eid/article/27/1/20-3281_article (19 October 2021).
Gesamtredaktion GIGA Focus
Redaktion GIGA Focus Lateinamerika
Lektorat GIGA Focus Lateinamerika
Regionalinstitute
Forschungsschwerpunkte
Wie man diesen Artikel zitiert
Drexler, Jan Felix, und Bert Hoffmann (2021), COVID-19 in Lateinamerika: wo wir stehen und was auf uns zukommt, GIGA Focus Lateinamerika, 5, Hamburg: German Institute for Global and Area Studies (GIGA), https://nbn-resolving.org/urn:nbn:de:0168-ssoar-75519-3
Impressum
Der GIGA Focus ist eine Open-Access-Publikation. Sie kann kostenfrei im Internet gelesen und heruntergeladen werden unter www.giga-hamburg.de/de/publikationen/giga-focus und darf gemäß den Bedingungen der Creative-Commons-Lizenz Attribution-No Derivative Works 3.0 frei vervielfältigt, verbreitet und öffentlich zugänglich gemacht werden. Dies umfasst insbesondere: korrekte Angabe der Erstveröffentlichung als GIGA Focus, keine Bearbeitung oder Kürzung.
Das German Institute for Global and Area Studies (GIGA) – Leibniz-Institut für Globale und Regionale Studien in Hamburg gibt Focus-Reihen zu Afrika, Asien, Lateinamerika, Nahost und zu globalen Fragen heraus. Der GIGA Focus wird vom GIGA redaktionell gestaltet. Die vertretenen Auffassungen stellen die der Autorinnen und Autoren und nicht unbedingt die des Instituts dar. Die Verfassenden sind für den Inhalt ihrer Beiträge verantwortlich. Irrtümer und Auslassungen bleiben vorbehalten. Das GIGA und die Autorinnen und Autoren haften nicht für Richtigkeit und Vollständigkeit oder für Konsequenzen, die sich aus der Nutzung der bereitgestellten Informationen ergeben.